Wednesday 24 July 2019
It was a very hot day, possibly the hottest of the summer so far, and I was feeling exhausted, sick and unstable – not good at all. The chemo from my latest inpatient stay had really hit me hard, much more than either of the previous cycles. I tried to sit outside a couple of times during the morning, but I didn’t last more than a minute or two in the heat before feeling quite unwell and needing to lie down in the shade.

One thing that sometimes helps with the feeling of sickness is eating something solid. As on many other mornings, Pia made me some porridge with organic berries and coconut milk, and that helped to settle my stomach a bit, for a little while at least.
I had an appointment for day chemo in the afternoon. Since my drug schedule had recently been messed up, having been a day behind my appointment schedule last week, I wanted to ensure that my Bleomycin for the afternoon’s session had been prepared for me before I made the trip to Bristol. My specialist nurse was off, so I couldn’t get hold of her. I tried to call the day chemo unit several times, but nobody was answering there. Eventually I spoke to someone from the chemo appointments team and they passed me onto one of the pharmacists. The pharmacist told me that I should be fine to come in for 3 pm, but she’d double check that my drugs had been prepared and would call me back if there were any issues.
I was feeling really rough and wasn’t coping too well. I really just wanted to curl up into a little ball and disappear for a while. However, I managed to take a shower, which I absolutely needed, and I got dressed.
Just before we left, I had a call from the pharmacist to say that there was actually a problem and that my drugs had not been prepared. It seemed that the dates on the drug charts in my patient notes had been updated, but this had not had the knock on effect of updating the pharmacy’s schedules accordingly. So twice now my chemo drugs had not been prepared in time for my appointments – I was glad I’d called ahead to check. Fortunately, the pharmacist said that she could have the Bleomycin prepared for me on an urgent basis, so I could still come in. If it wasn’t ready for 3 pm, it would be sometime soon after, which was fine given that it wouldn’t normally be infused until almost an hour after my appointment began.
I felt pretty awful during the car journey, worse than on any other journey we’d made during my chemotherapy. The heat didn’t help, even though we had cool air pumping through the vents. I started to feel what was probably the closest to proper nausea I’d had so far. For the first time during my chemo treatment, I felt as though I might actually have to vomit and held onto a plastic bag, just in case.
Pia dropped me off at the BHOC entrance, as I wasn’t going to be able to walk very far and we usually had to park a fair distance away. I walked up to the day chemo reception desk where I had to lean on the counter and clearly must have looked a wreck, as the receptionist had to ask how I was feeling and if I was ok. I sat in the waiting area for a few minutes, most of the time leaning forward with my elbows on my knees.
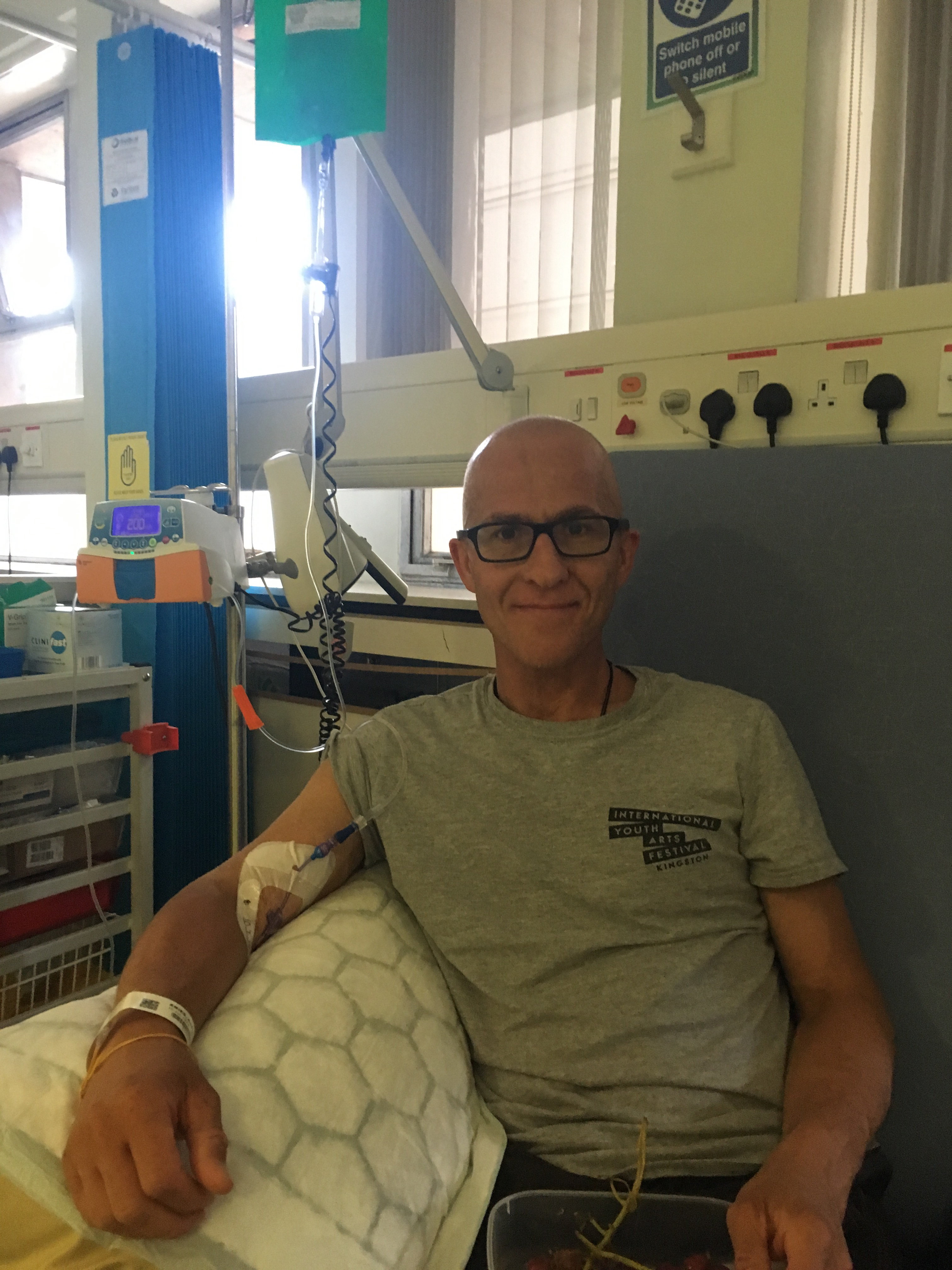
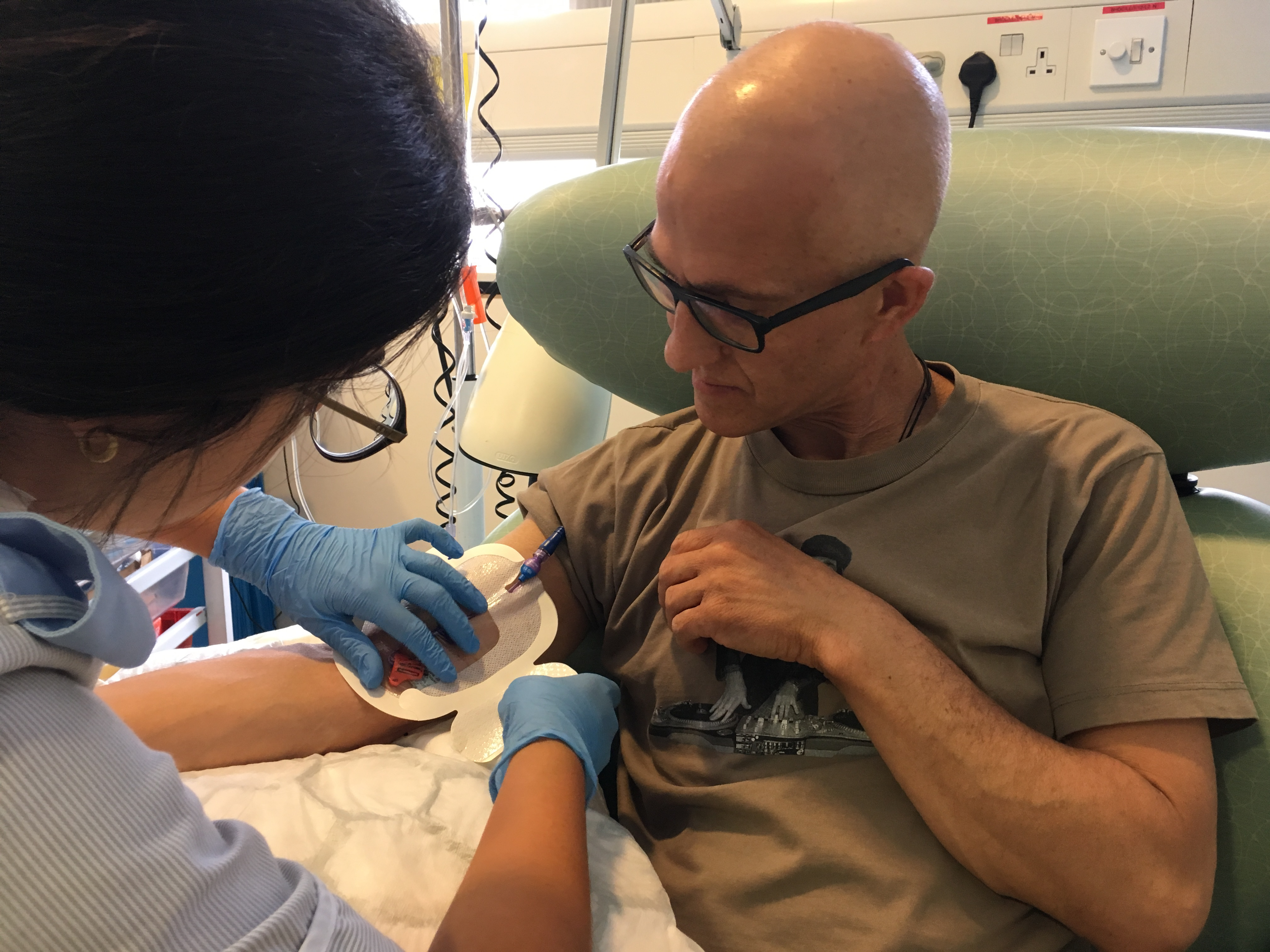
When my chemo nurse came to collect me, I told her how horrible I was feeling. As I wasn’t feeling good, she wanted to check a few things before starting any treatment. She took my blood pressure, pulse and temperature, which were all ok, and she asked me a number of questions. She also wanted to make sure that I felt capable of seeing through the day’s session before we commenced. I just wanted to get it done. I had my PICC line redressed and some blood was taken to check my full blood count. Everything on the FBC came back looking alright.
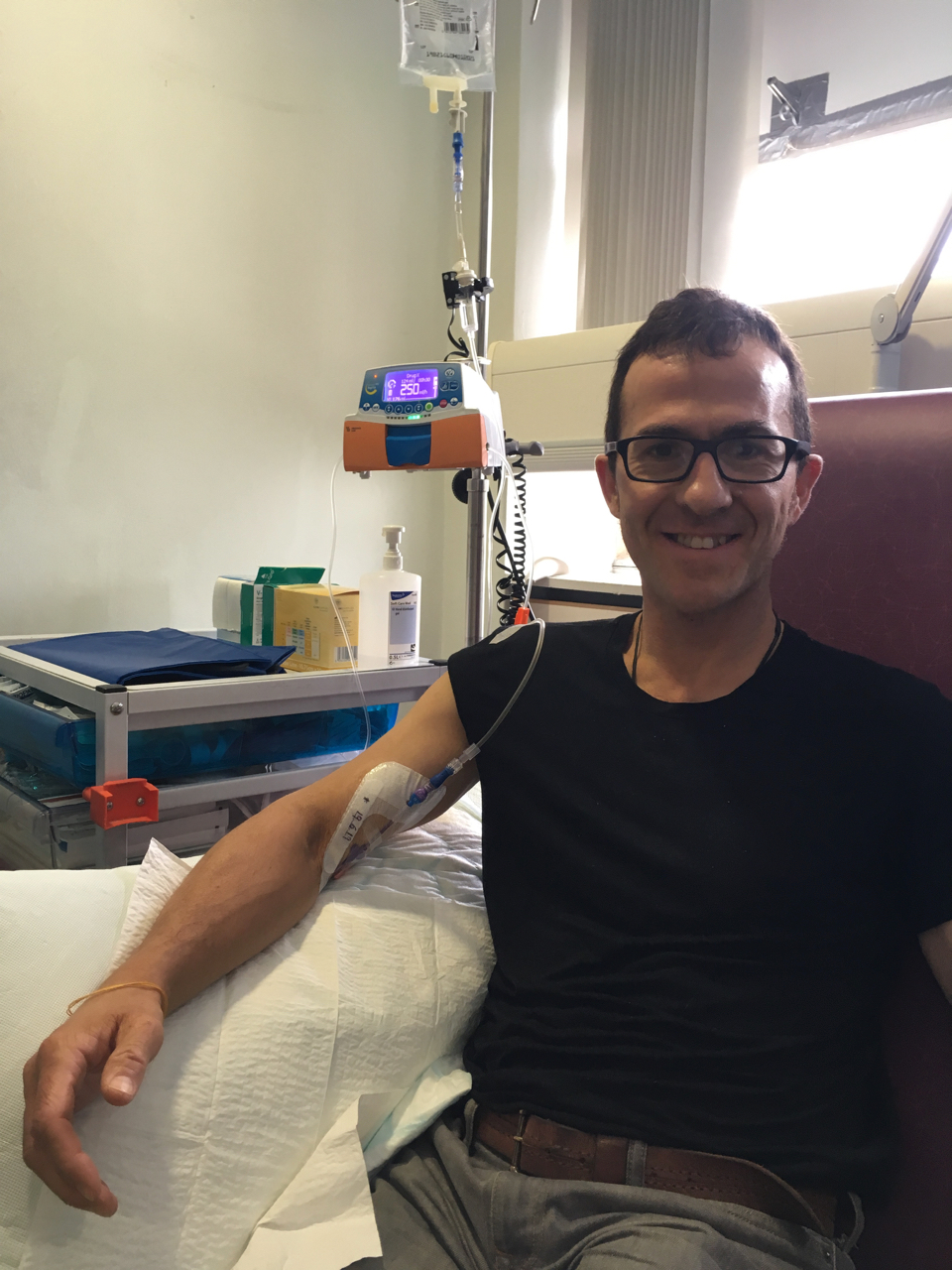
It was cooler inside the hospital and I started to feel a bit less unwell after being sat there for a while. After Pia arrived, having parked the car, I was hooked up to an IV pump and got started on some saline and hydrocortisone. I spent most of the next hour with my eyes closed, not quite asleep, but not far off. I just sat back as still as possible. After half an hour, I started the Bleomycin, which infuses over 30 minutes. Then I had 15 minutes more of saline, after which I was able to leave.
By this point I was feeling much improved on when I’d arrived, but still pretty poor. Fortunately it had cooled down a little outside. I waited by the hospital entrance while Pia fetched the car, then we drove home. The drive home felt a lot easier than the earlier drive to the hospital.
When we got home, I lay down in bed. I’m not sure that I actually slept, but it was close enough. I came downstairs in the evening and we ate on the sofa before going to bed.
As per day 9 of cycles 1 & 2, my temperature did rise a bit during the evening, a known side effect of Bleomycin. When I went to bed, it was about 37.5 C, having risen from closer to 36 C. It then went up to almost 38 C, but had come down again when we checked it later during the night (Pia had set alarms so that we could wake and check it every so often). Other than for waking to check my temperature, I slept quite well.
This had been the hardest day so far and I’d felt awful all day, but particularly during the trip to the hospital. I think this was all the cumulative effect of the chemo drugs in my system, really hitting me hard. I did wonder how long this would last and how much worse it could get, but it was no good dwelling on such things. I’d have to take each day as it comes.